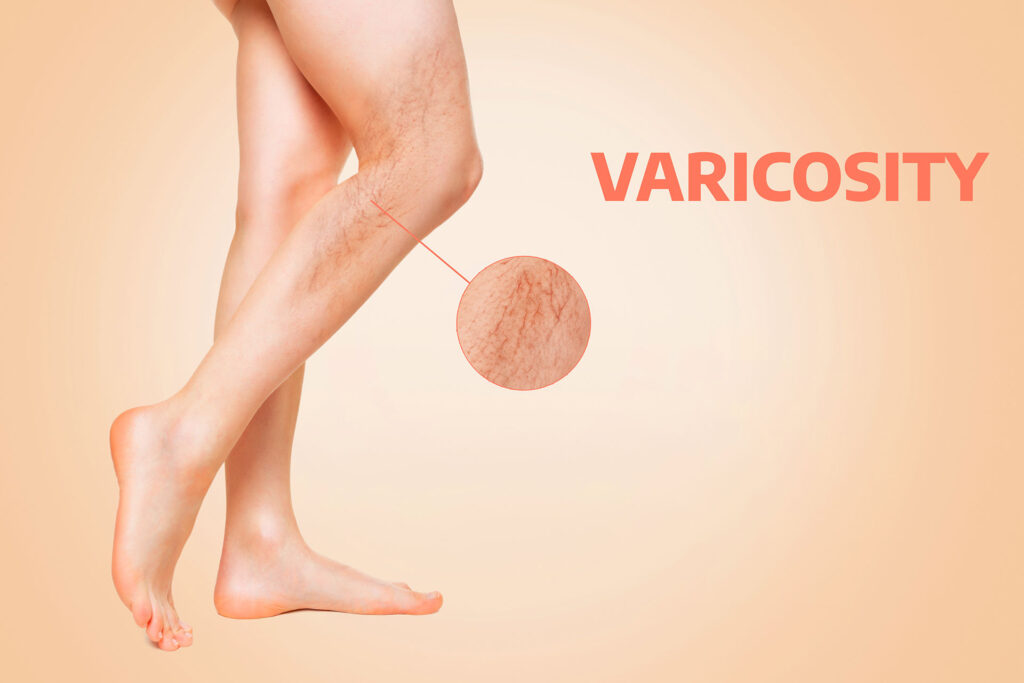
If you’ve ever glanced down at those bulging, twisted veins on your legs and wondered, “Should varicose veins be painful?” You’re not alone. Millions of people struggle with this common vascular condition, often dismissing the discomfort as a normal part of aging or a long day on their feet. But here’s the truth: while some varicose veins are merely a cosmetic concern, painful varicose veins are a clear signal from your body that something needs attention.
Should Varicose Veins Be Painful? The Short Answer
Varicose veins can be painful, but they shouldn’t be. Pain is your body’s way of telling you that the underlying venous insufficiency has progressed beyond a simple cosmetic issue. While many people experience varicose veins without noticeable pain initially, persistent or worsening discomfort suggests that the affected veins are no longer functioning properly.
Healthy veins efficiently return blood from your legs back to your heart. When the one-way valves inside these veins weaken or fail, blood pools in the lower extremities, causing the veins to enlarge, twist, and become visible beneath the skin. This pooling and pressure are what often lead to pain and other troubling symptoms.
Common Symptoms of Painful Varicose Veins
Varicose vein pain doesn’t always present as sharp, stabbing discomfort. In fact, the sensations can vary widely from person to person. Recognizing these symptoms early is key to seeking timely treatment.
- Aching or throbbing in the legs, especially after standing or sitting for long periods
- Heaviness or fatigue in the legs at the end of the day
- Burning or itching sensations around the affected veins
- Muscle cramps, particularly at night
- Swelling in the lower legs and ankles
- Tenderness when touching the veins
- Skin discoloration or changes in texture near the affected area
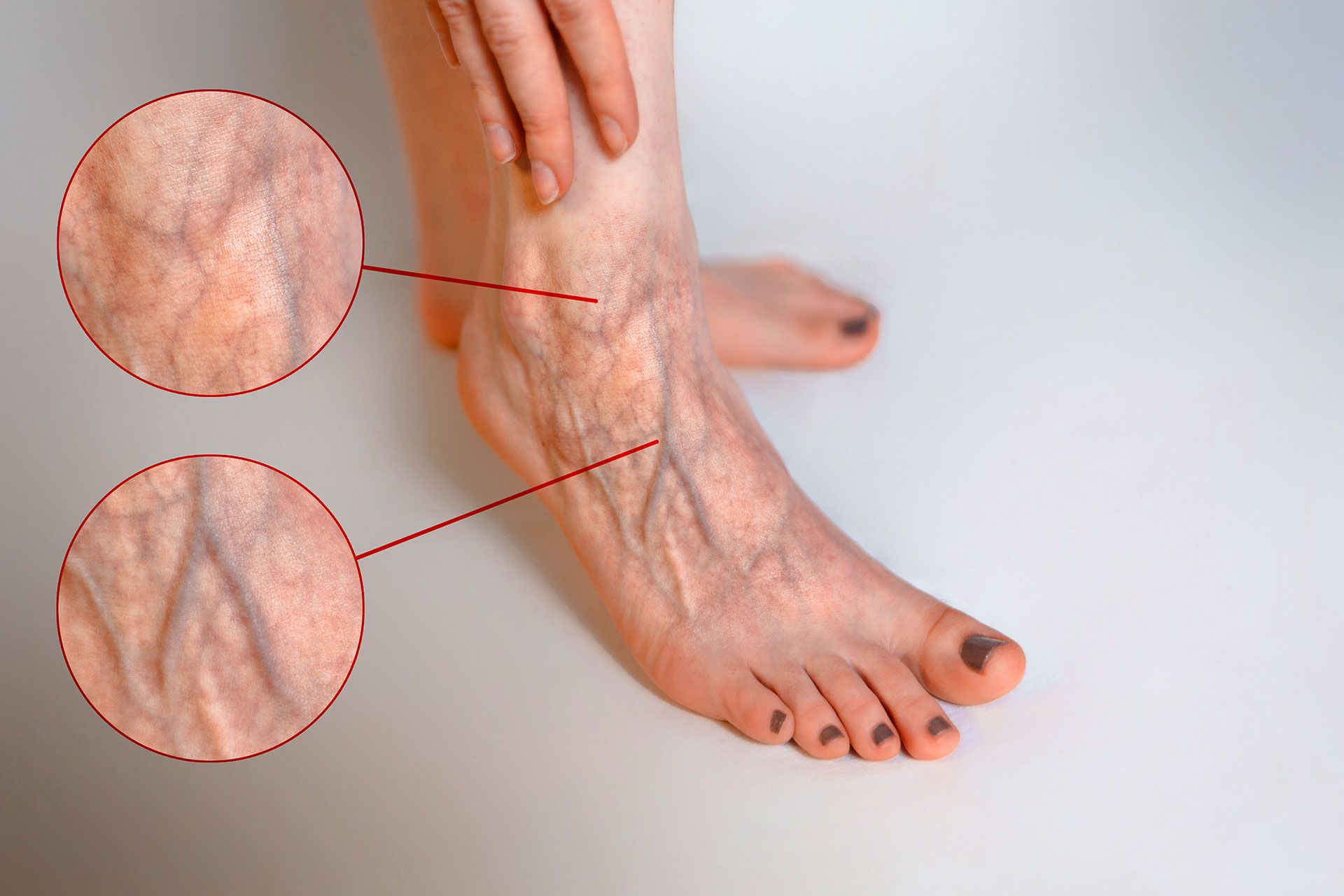
Why Do Varicose Veins Cause Pain?
The pain associated with varicose veins stems from chronic venous insufficiency, a condition where damaged valves allow blood to flow backward and pool in the veins. This pooling creates increased pressure within the vessel walls, leading to inflammation, swelling, and nerve irritation.
As the condition progresses, the surrounding tissues can become starved of proper circulation, leading to deeper, more persistent aches. Some patients also experience nerve pain that overlaps with other conditions, making accurate diagnosis essential.
The Connection Between Vein Issues and Leg Discomfort at Night
Many people with varicose veins report increased discomfort during the evening hours, with symptoms intensifying when they try to sleep. This nighttime leg discomfort can sometimes be confused with, or coexist alongside, Restless Legs Syndrome, a neurological condition that creates an irresistible urge to move the legs. Understanding the difference between these conditions and how vascular health may contribute to both is crucial for getting the right treatment.
When Should You Worry About Varicose Vein Pain?
Not all varicose vein pain is created equal. Mild discomfort after a long day might be manageable with rest and elevation, but certain warning signs indicate that professional evaluation is necessary.
Red Flags That Require Medical Attention
- Persistent pain that doesn’t improve with rest, elevation, or over-the-counter pain relievers
- Open sores or ulcers near the ankle that won’t heal
- Bleeding from a varicose vein
- Hardening or thickening of the skin around the vein
- Sudden swelling in one leg
- Warmth and redness along the vein, which may indicate phlebitis
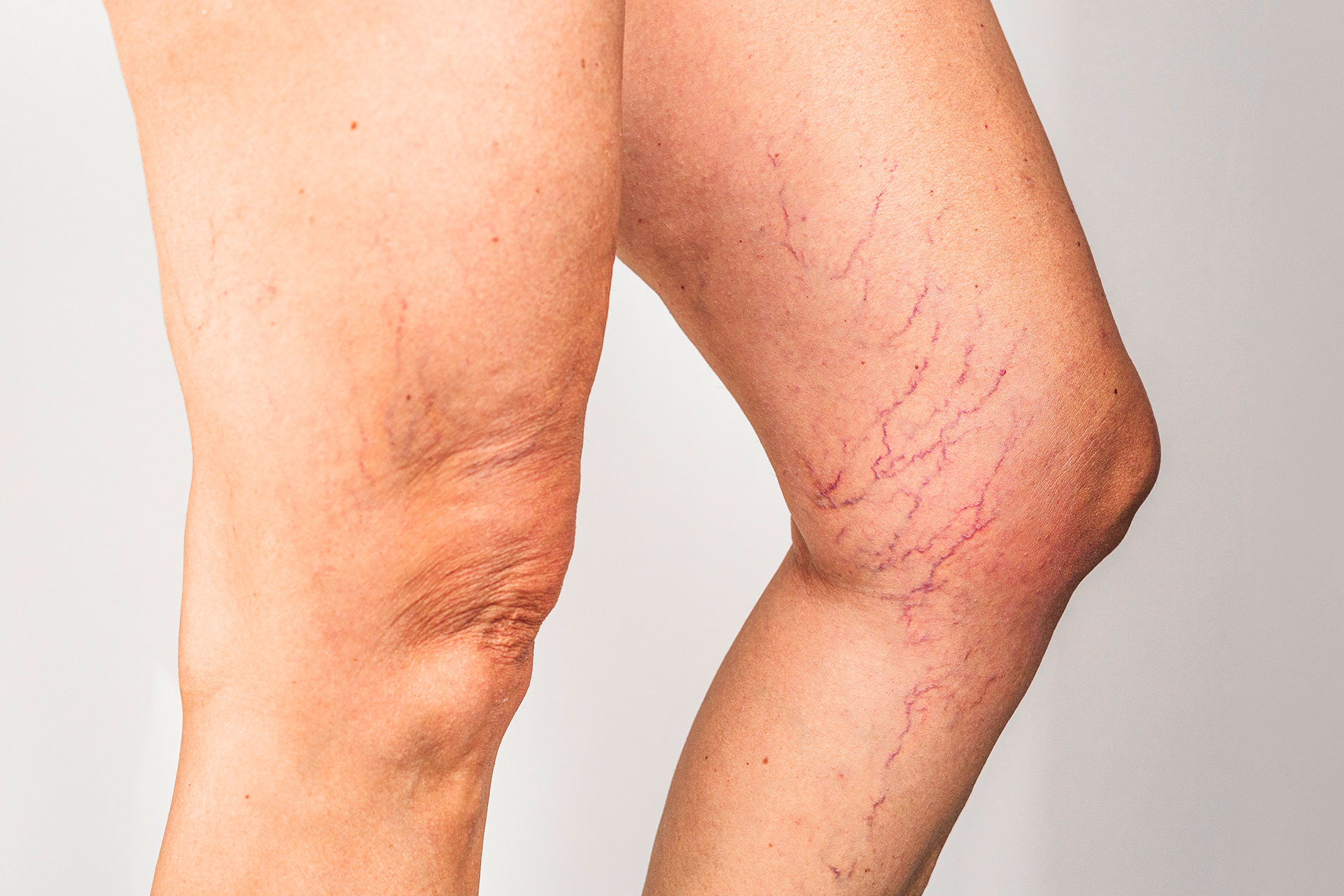
Risk Factors That Increase Pain Severity
Certain factors can make varicose veins more likely to become painful or worsen existing discomfort. Knowing these risk factors helps you take preventive action.
- Age: Vein valves naturally weaken over time
- Genetics: A family history of varicose veins significantly raises your risk
- Pregnancy: Hormonal changes and increased blood volume strain the veins
- Prolonged standing or sitting: Common in occupations like nursing, teaching, or office work
- Obesity: Excess weight puts additional pressure on leg veins
- Hormonal changes: Birth control, menopause, and hormone therapy can affect vein health
Effective Ways to Manage and Treat Painful Varicose Veins
The good news is that painful varicose veins are highly treatable. Modern vein treatments are minimally invasive, performed in-office, and require little to no downtime, a far cry from the painful vein-stripping surgeries of the past.
Conservative At-Home Strategies
For mild symptoms, lifestyle modifications can offer significant relief:
- Elevate your legs above heart level for 15 minutes several times a day
- Wear compression stockings to support healthy circulation
- Exercise regularly, walking, swimming, and cycling promote blood flow
- Maintain a healthy weight to reduce pressure on your veins
- Avoid prolonged standing or sitting, take breaks to move every 30 minutes
- Stay hydrated and eat a fiber-rich diet to prevent constipation, which can worsen vein pressure
Medical Treatment Options
When at-home measures aren’t enough, several minimally invasive procedures can effectively eliminate painful varicose veins:
- Endovenous Laser Ablation (EVLA): Uses laser energy to close off damaged veins
- Radiofrequency Ablation (RFA): Employs heat from radiofrequency waves to seal veins
- Sclerotherapy: Involves injecting a solution that causes the vein to collapse and fade
- VenaSeal: Uses medical adhesive to seal problematic veins
- Ambulatory Phlebectomy: Removes surface varicose veins through tiny incisions
Don’t Ignore Painful Varicose Veins
Untreated varicose veins rarely improve on their own, and the pain often worsens over time. More importantly, neglecting symptoms can lead to serious complications such as venous ulcers, deep vein thrombosis (DVT), or chronic venous insufficiency. Early intervention not only relieves pain but also prevents these potentially dangerous outcomes.
When to See a Vein Specialist
If your varicose veins are causing pain, interfering with daily activities, disrupting your sleep, or affecting your quality of life, it’s time to consult a board-certified vein specialist. A thorough evaluation, typically including a duplex ultrasound, can identify the underlying cause of your symptoms and determine the most effective treatment approach.
Your Pain Is a Message, Listen to It
So, should varicose veins be painful? While many people experience some level of discomfort, persistent pain is never normal and shouldn’t be ignored. Whether it’s a dull ache, burning sensation, or throbbing that keeps you up at night, your body is telling you that something is wrong with your venous system.
The encouraging news is that today’s vein treatments are safer, faster, and more effective than ever before. By recognizing the symptoms early, understanding the risk factors, and seeking professional care, you can eliminate painful varicose veins for good and reclaim the comfort and confidence you deserve. Don’t let painful veins dictate your life; take the first step toward healthier legs today.