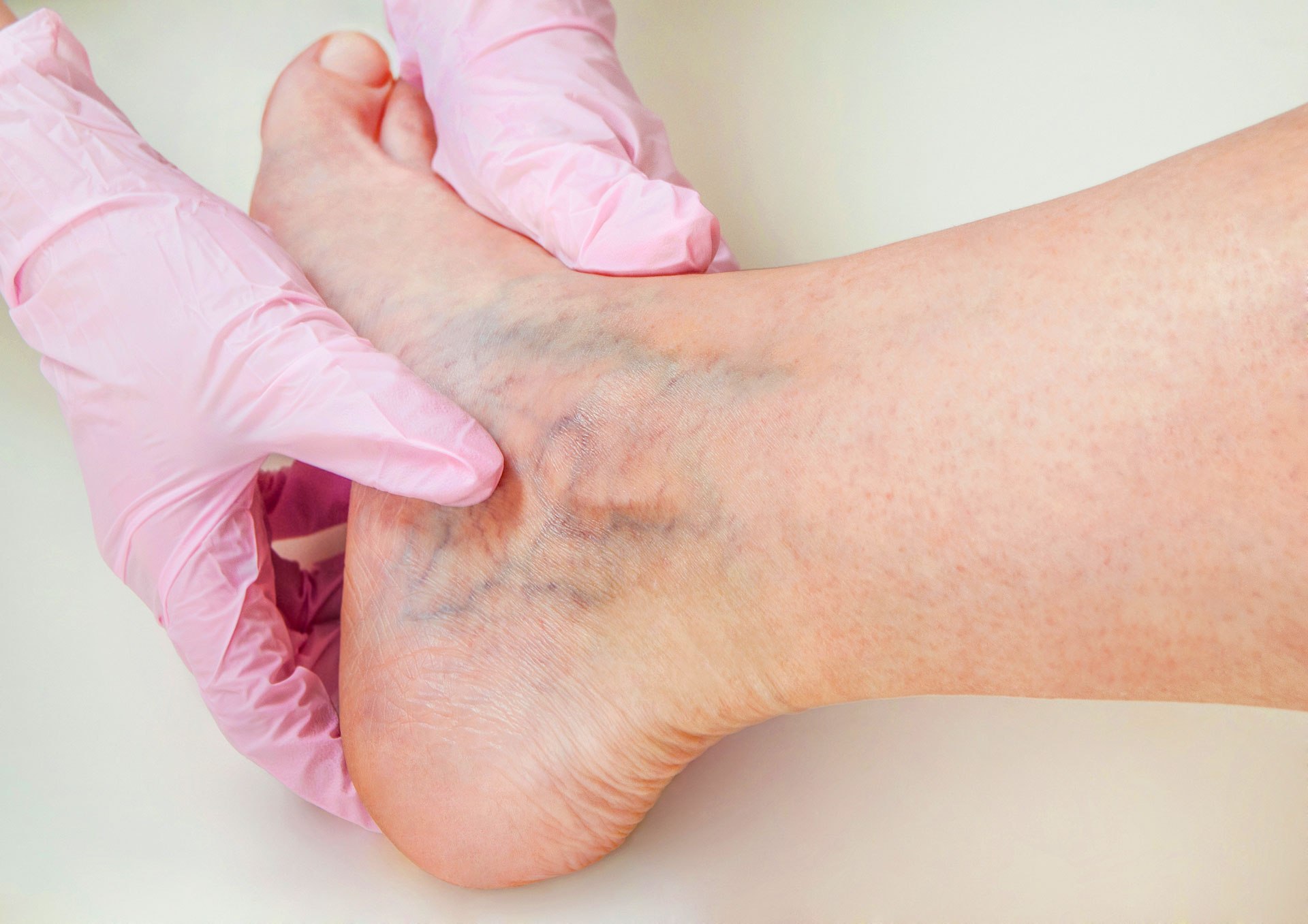
What is restless legs syndrome?
Restless legs syndrome (RLS), also called Willis-Ekbom disease, is a neurological condition that creates an overwhelming urge to move the legs, paired with uncomfortable sensations like crawling, throbbing, or burning beneath the skin. Symptoms of restless legs syndrome worsen during rest and peak at night, making it both a sleep disorder and a movement disorder.
What many people do not realize is that RLS is frequently tied to poor venous circulation. When vein valves weaken and blood pools in the lower legs, the resulting pressure and nerve irritation can generate the restlessness that disrupts sleep night after night. For patients dealing with chronic leg pain, identifying and treating that underlying vein condition often produces dramatic, lasting relief.
Recognizing the symptoms of restless legs
Four hallmark features separate RLS from ordinary leg fatigue or cramps. People describe the feeling as crawling, pulling, burning, or an electric current deep beneath the skin:
In more severe cases, restless legs syndrome symptoms can spread to the arms. About 80% of RLS patients also experience involuntary limb jerking during sleep, disrupting rest and causing chronic daytime fatigue.
What is your body lacking when you have restless legs?
Nutritional deficiencies and poor circulation are often at the core of why RLS develops.
The brain relies on iron to regulate dopamine. Even patients within “normal” lab ranges may have ferritin too low for healthy nerve function. Specialists recommend ferritin above 75 ng/mL for RLS patients.
Damaged vein valves allow blood to pool in the lower legs. That pooling creates pressure, irritates surrounding nerves, and generates the crawling sensations that define RLS. Treating the leg vain condition often resolves the restlessness entirely.
Low magnesium increases nerve excitability, closely linked to the leg cramps at night that frequently overlap with RLS. Vitamin D deficiency is also observed more often in RLS patients.
What causes restless legs syndrome?
Weakened vein valves cause blood to pool in the lower legs, creating the nerve pressure that drives RLS sensations and nighttime restlessness.
Nearly half of RLS patients have a first-degree relative with the condition. A genetic predisposition to both RLS and vein disease is well-documented.
Low iron disrupts dopamine regulation. Even patients without anemia may have brain iron levels too low for proper nerve and movement control.
Kidney disease, diabetes, peripheral neuropathy, and pregnancy all increase the risk of developing or worsening secondary RLS symptoms.
What is the best treatment for restless legs?
When vein disease is identified as a contributing cause, treating the circulation problem often produces dramatic relief. CURA Vein Centers offer minimally invasive, in-office treatments with no surgery and no downtime. See the spider vein treatments that deliver lasting results.
Lifestyle strategies that support relief
Fixed wake times and a cool, dark bedroom stabilize the circadian rhythm that governs when RLS symptoms intensify each night.
Daily walking improves circulation and reduces symptom frequency. Avoid intense exercise close to bedtime, which can worsen restlessness.
Applying heat and gentle pressure before bed quiets the urge to move and eases the transition into sleep considerably.
Both substances lower the threshold for RLS symptoms in the evening. Even a moderate reduction often produces a noticeable difference in sleep quality.
Frequently asked questions
Is RLS the same as leg cramps? +
No. Leg cramps are sudden, painful muscle contractions that pass quickly. Restless legs syndrome involves crawling or pulling sensations with an urge to move. Walking typically relieves RLS temporarily but does not resolve a muscle cramp in the same way.
Can vein disease really cause restless legs? +
Yes. Venous insufficiency, where damaged vein valves allow blood to pool in the legs, creates pressure and nerve irritation that directly contributes to RLS symptoms. Treating the vein condition often reduces or eliminates the restlessness entirely.
Can RLS go away on its own? +
Secondary RLS caused by iron deficiency or venous disease often improves once the underlying issue is addressed. Primary RLS tends to be chronic but fluctuates in severity, with some people experiencing extended periods of mild or no symptoms.
When should I see a specialist? +
If RLS symptoms are disrupting your sleep, affecting your daily function, or getting progressively worse, a vein and pain specialist can evaluate whether venous insufficiency is involved. Early care consistently leads to better outcomes.