A cluster of purple veins on legs that was not there before. A dull ache that builds through the day. Swelling that does not go away. These signs are easy to dismiss, but vein conditions in the leg are more common than most people realize, and ignoring them can allow a manageable problem to become a serious one.
Anatomy Veins of the Leg: The Basics
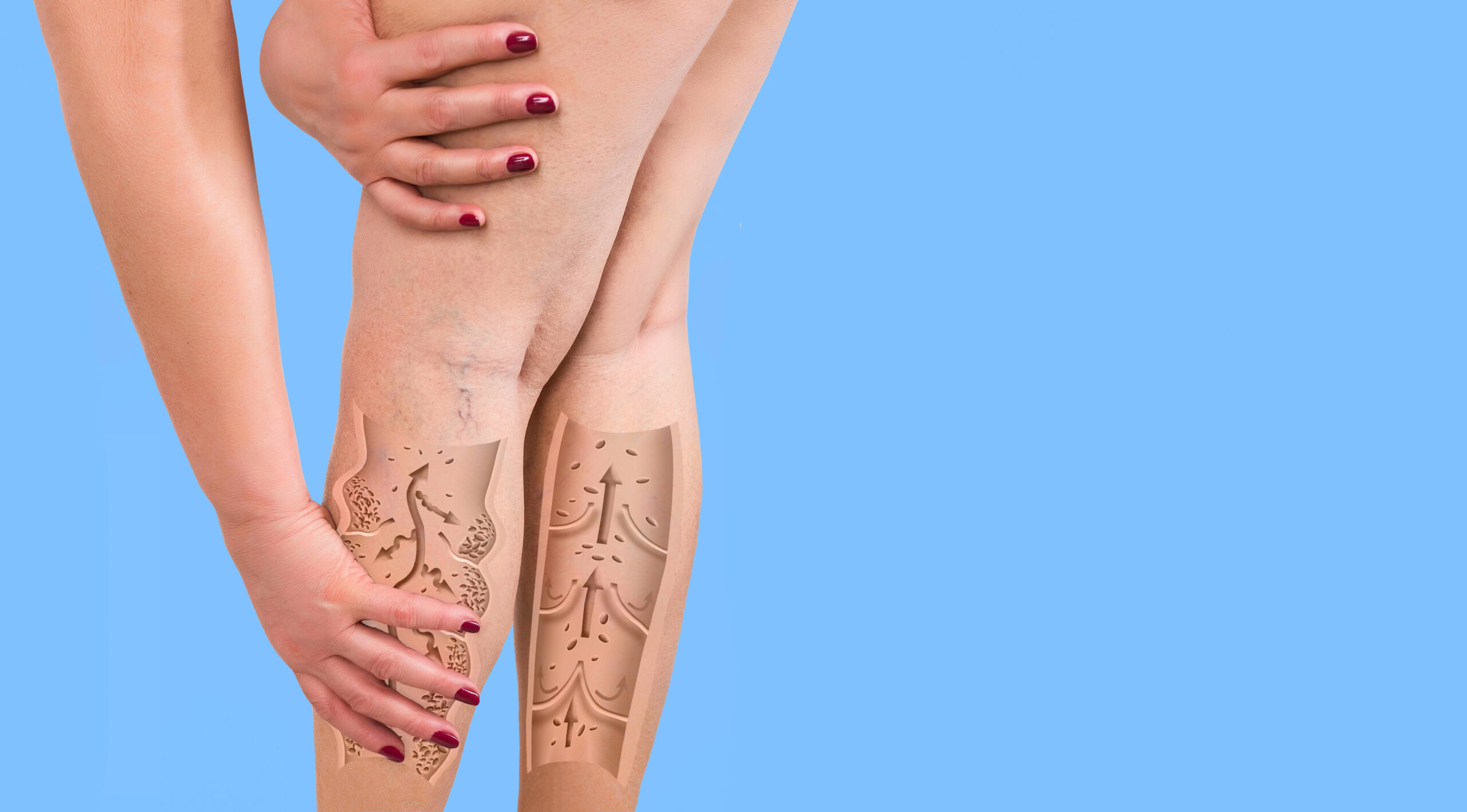
The leg has two venous systems. The deep system runs through muscle tissue and carries most blood back to the heart. The superficial system sits closer to the skin and connects to the deep system through perforating veins. Both rely on one-way valves to push blood upward against gravity.
When those valves weaken, blood pools. That pooling is the root cause of most vein conditions in the leg, from minor spider veins to chronic venous insufficiency.

Common Vein Conditions in the Leg
Spider Veins
Small, web-like vessels near the skin surface. Purple veins on legs of this type are usually painless but can itch or cause mild burning. They are caused by minor valve dysfunction or increased local pressure. Several effective spider vein treatments are available if they are spreading or causing symptoms.
Varicose Veins
Larger, rope-like veins that bulge visibly beneath the skin. They develop when superficial vein valves fail, causing blood to accumulate and the vein wall to stretch. Symptoms include aching, heaviness, and itching. Without treatment, varicose veins can progress to skin changes and ulcers.
Chronic Venous Insufficiency
When valve failure becomes persistent, blood pools continuously in the lower leg, causing veins swelling in leg, skin discoloration, and in advanced cases, wounds that are slow to heal. CVI often requires medical management rather than lifestyle changes alone.
Deep Vein Thrombosis
A clot in the deep veins of the leg, usually the calf or thigh. Symptoms include sudden swelling, warmth, redness, and pain. DVT is a medical emergency because the clot can travel to the lungs.
You experience sudden swelling in one leg with pain or warmth. Do not wait to see if it resolves.
Symptoms Worth Paying Attention To
- Aching or heaviness that worsens after prolonged standing or sitting
- Veins swelling in leg, especially around the ankles by late afternoon
- Itching or burning along a visible vein
- Purple veins on legs that are new, growing, or spreading
- Skin near the ankle that has become discolored or thickened
- Frequent leg cramps, particularly at night
Night cramps are more connected to vein health than many people realize. If they are a regular occurrence, nocturnal cramps may be worth investigating in the context of your vein health overall.
Leg With Veins: When to Take It Seriously
A leg with veins that are visibly enlarged is not always in medical danger, but some situations do warrant prompt attention:
- Sores or ulcers near the ankle that are slow to heal
- A vein that becomes suddenly hard, red, or tender
- Bleeding from a varicose vein
- Swelling that does not improve with rest or elevation
In some cases, vein-related nerve compression leads to chronic pain that goes beyond the vein itself. When that happens, nerve pain management may become part of the care plan alongside vein treatment.
What Treatment Looks Like
Treatment depends on the type and severity of the condition. Most modern vein procedures are minimally invasive, performed in an outpatient setting, and require little to no downtime.
Lifestyle and Conservative Measures
For mild symptoms, the first step is usually conservative management. Graduated compression stockings reduce pooling by applying gentle pressure to the leg. Regular walking activates the calf muscle pump and improves venous return. Elevating the legs when resting, maintaining a healthy weight, and avoiding prolonged sitting or standing all help slow progression and ease discomfort. These measures manage symptoms but do not repair existing valve damage.
Sclerotherapy
A chemical solution is injected directly into the affected vein, causing it to scar and close. Blood is then rerouted through healthier vessels. Sclerotherapy is the standard treatment for spider veins and smaller varicose veins. It requires no anesthesia, takes around 30 minutes, and most people return to normal activity the same day.
Thermal Ablation
Radiofrequency ablation (RFA) and endovenous laser ablation (EVLA) use heat delivered through a thin catheter inserted into the vein to close it from the inside. Both are highly effective for larger varicose veins and chronic venous insufficiency, with success rates consistently above 90 percent. The procedure is done under local anesthesia and takes under an hour.
Phlebectomy
For surface varicose veins that are too large for sclerotherapy but do not require full ablation, ambulatory phlebectomy is an option. Tiny incisions are made along the vein and it is removed in sections. The incisions are small enough that stitches are rarely needed.
FAQ: Leg With Veins
Concerned about what you are seeing or feeling in your legs? Our specialists can help you understand your options.


