Why Teachers Get Varicose Veins
More Than Most People
Indeed, most educators notice the signs gradually: a dull ache at the end of the day, legs that feel heavy on the commute home, or visible blue-green cords appearing along the calves. In many cases, by the time these symptoms become truly disruptive, the underlying vein damage has already been building for years.
With that in mind, this article explains exactly why teaching is so hard on veins, what the warning signs look like, and what modern, minimally invasive options now make relief straightforward and fast.
The Vein Problem with Standing All Day
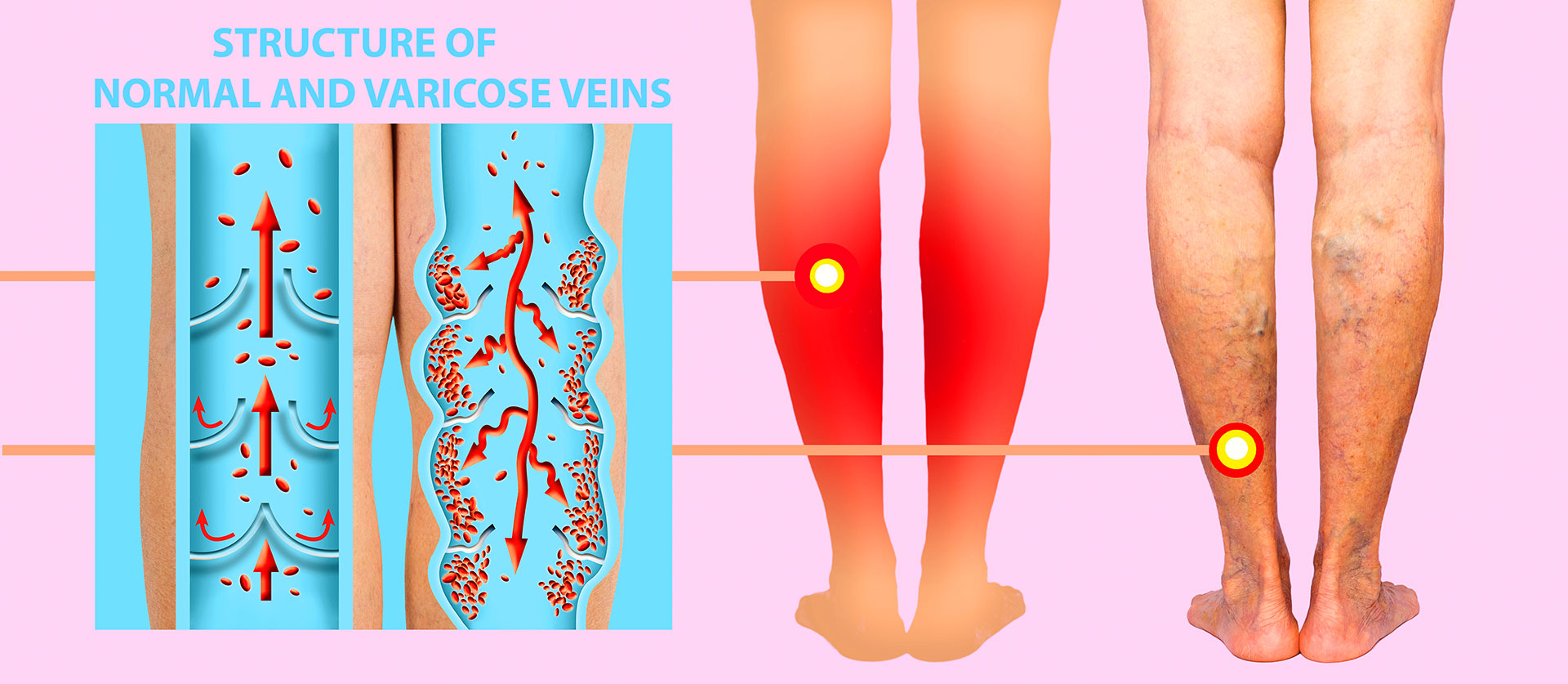
To understand why teachers are so vulnerable, it helps to first understand how leg veins actually work. Unlike arteries, which rely on the heart's pumping force to move blood, veins in the legs must push blood upward against gravity, relying on a series of one-way valves and the contraction of surrounding calf muscles.
When you walk, your calf muscles compress the veins with each step, propelling blood upward toward the heart. When you stand still for long periods, however, that muscle pump becomes entirely idle. As a direct consequence, blood begins to pool in the lower leg veins, steadily increasing internal pressure on the vessel walls with every passing hour.
Over time, this repeated pooling gradually weakens vein walls and stretches the delicate valves that keep blood flowing in one direction. Once those valves fail, a condition known as venous reflux, blood flows backward and consequently pools even more aggressively. As a result, the vessels enlarge, twist, and bulge visibly under the skin, causing the pain and discomfort most people recognize as varicose veins.
Why Teachers Specifically Are at Higher Risk
Most professions involve a natural mix of sitting, standing, and walking. Teaching, by contrast, demands prolonged static standing, often on hard concrete or tile floors, with very limited opportunity to sit, elevate the legs, or move freely through the room. Furthermore, several factors specific to the classroom environment compound this risk and make vein damage even more likely over time.
Key Risk Factors for EducatorsHow Teaching Compares to Other High-Risk Jobs
Teachers often do not recognize themselves as a high-risk group, partly because the conversation around varicose veins tends to center on nurses or surgeons. Nevertheless, the underlying mechanism is identical in all cases: sustained upright standing with limited calf muscle activity. As the table below illustrates, teachers rank directly alongside the most at-risk professions.
| Occupation | Daily Standing Hours | Static vs. Active Standing | Varicose Vein Risk |
|---|---|---|---|
| Teacher | 6–8 hours | Mostly static | High |
| Nurse / Surgeon | 8–12 hours | Mixed | High |
| Retail Worker | 6–8 hours | Mixed | High |
| Chef / Kitchen Staff | 8–10 hours | Mixed | High |
| Office Worker | 1–2 hours | Minimal | Moderate |
"Varicose veins in teachers are not a cosmetic inconvenience. They are the predictable result of years of sustained venous pressure, and they deserve the same clinical attention given to any occupational injury."
Warning Signs Teachers Should Not Ignore
Because symptoms build gradually over years, many teachers normalize their discomfort as a routine part of the job. The signs below, however, indicate vein damage that is likely to worsen without treatment. In addition, the earlier that treatment begins, the simpler it tends to be.
This is a hallmark of venous insufficiency. If your legs feel noticeably worse by 3pm than they did at 8am, it is because venous pressure has been building for hours. For this reason, even this symptom alone warrants a vein evaluation.
Swelling that appears in the afternoon and eases overnight, only to return each school day, indicates that venous pressure is high enough to push fluid into surrounding tissues.
Twisted, rope-like veins visible beneath the skin are a definitive sign of valve failure. Specifically, their presence confirms that blood is being trapped under pressure inside diseased vessel segments, and treatment should not be postponed.
An irresistible urge to move the legs during rest, particularly in the evenings, is frequently linked to underlying venous insufficiency. In fact, many patients report significant improvement in restless leg symptoms after vein treatment.
Brownish or reddish discoloration near the ankle signals that red blood cells are leaking from overpressured veins into surrounding tissue. Because this indicates sustained, advanced vein damage, it demands prompt evaluation without delay.
Practical Steps Teachers Can Take Now
While the only permanent solution for failing vein valves is a medical procedure, the following measures can nonetheless reduce daily venous pressure and help slow the progression of damage in the meantime.
These measures help manage symptoms effectively, yet it is important to be clear: they do not correct the underlying vein valve damage. Therefore, if varicose veins are already present, or if symptoms are limiting your daily comfort, a consultation with a specialist is the essential next step. A vein specialist can then assess your venous health with a painless duplex ultrasound and outline the best path forward.
What Treatment Options Are Available
The good news for teachers is that modern vein treatment has changed dramatically. Gone are the days of surgical stripping, hospital stays, and weeks of recovery. Today, instead, procedures are minimally invasive, performed in-office under local anesthetic, and allow most patients to return to the classroom within a day or two.
Since vein conditions vary, the right approach depends on the size and location of the affected vessels. Your specialist will assess this during a duplex ultrasound and may recommend one of the following options:
Minimally Invasive Procedures Your Specialist May Recommend
A thin catheter delivers controlled heat energy along the diseased vein, causing it to collapse and seal shut permanently. As a result, blood reroutes through healthy surrounding veins. Notably, RFA carries a success rate above 92% and allows same-day return to normal activity. Moreover, it is one of the most widely used procedures for larger varicose veins. Learn about RFA.
A medical solution is injected directly into the diseased vein, causing it to scar and close. This approach is particularly effective for smaller varicose veins and spider veins. Furthermore, multiple veins can be treated in a single session, and no anesthesia is required. In fact, most patients see noticeable results within just a few weeks.
A specially formulated medical adhesive is delivered into the damaged vein, bonding the vessel walls together permanently. Unlike RFA, VenaSeal requires no heat, no tumescent anesthesia, and no compression stockings post-procedure, making it one of the most comfortable options available.
A rotating catheter tip combines mechanical disruption of the vein wall with chemical sclerosant, achieving closure without thermal energy. It is therefore an excellent option for patients who cannot tolerate the tumescent injections used in RFA. For a broader comparison of these approaches, this overview of top vein treatments is a useful starting point.
"You do not need to schedule time off for vein treatment. Most teachers have their procedure on a Friday and are back in the classroom on Monday."
Ready to Take the First Step?
A duplex ultrasound is all it takes to assess your vein health and determine whether treatment is the right next step. In most cases, the consultation is straightforward, painless, and covered by insurance when symptoms are present.
Book a Consultation →