Achy Legs on a Monday?
It's Not Just the Weekend
vein disease
blame lifestyle
instead
In most cases, this pattern repeats itself week after week, slowly intensifying over months and years. With that in mind, this article explains exactly why your legs ache the way they do, what the warning signs look like, and what modern treatment options can provide lasting relief.
Why the Workweek Punishes Your Veins
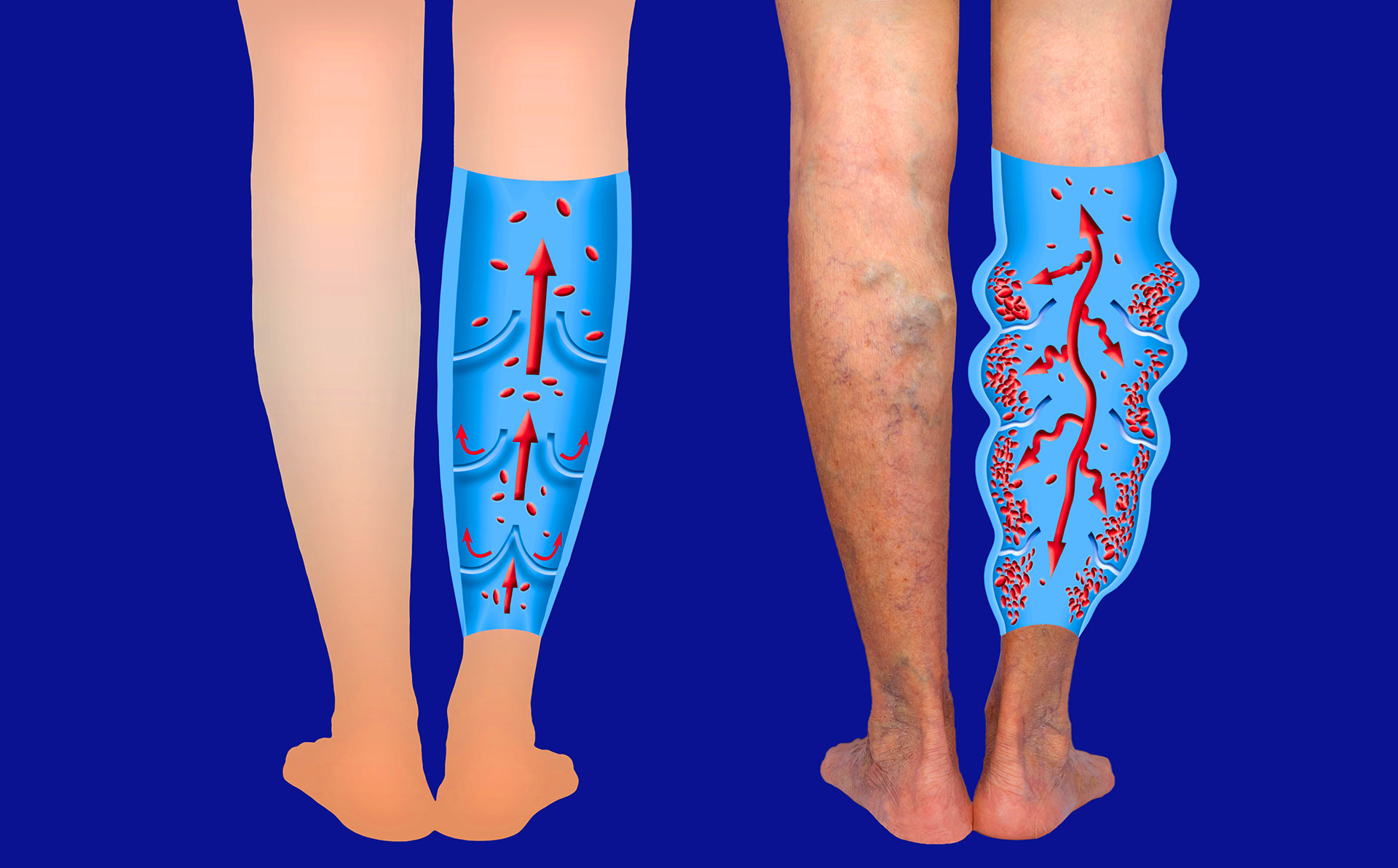
To understand the Monday pattern, it helps to first understand how venous pressure builds over time. Unlike arteries, which rely on the heart's pumping force, leg veins must push blood upward against gravity using a series of one-way valves. When those valves are healthy, blood flows efficiently back to the heart with every step you take.
However, when vein valves weaken or fail, a condition called venous reflux, blood flows backward and begins pooling in the lower legs. As a direct consequence, pressure inside the vein walls builds with every hour you spend upright, whether standing or sitting. Consequently, by Friday afternoon, that accumulated pressure has been compounding for five full days.
Although the weekend provides some respite, the valve damage itself does not resolve. Therefore, when Monday arrives, your veins are resuming the cycle in a weakened state. That is why the aching feels sharpest at the start of the week rather than at the end, and why it is a pattern worth taking seriously.
before the weekend
to repair valve damage
degree of venous disease
The Weekly Pattern That Points to Your Veins
Not all leg pain is vein-related. Muscle soreness from exercise, for example, is expected and resolves predictably within a day or two. Vein-related leg aching, however, follows a much more consistent and recognizable cycle. Understanding this distinction is therefore an important first step toward getting the right diagnosis.
How Vein-Related Aching DiffersWarning Signs You Should Not Dismiss
Because vein disease progresses gradually, many people adapt to their symptoms rather than seeking help. The signs below, however, indicate damage that is likely to worsen without treatment.
-
01Aching or Heaviness That Builds Through the DayA progressive worsening of discomfort from morning to evening is the most consistent symptom of venous insufficiency. Specifically, if your legs feel measurably worse by afternoon than they did at the start of the day, venous pressure is the most likely cause.
-
02Ankle and Foot SwellingSwelling that appears during the day and eases after sleep is a hallmark of elevated venous pressure. In addition, shoes that feel tighter in the afternoon than in the morning are a reliable early indicator worth investigating.
-
03Visible Varicose or Spider VeinsBulging, rope-like veins or a spreading network of spider veins confirm that vein valve failure is already present and that proper evaluation is warranted.
-
04Itching or Burning SkinA persistent itch or burning sensation near the calf or ankle indicates that blood is pooling close to the skin surface — a consistently overlooked yet reliable sign of venous disease.
-
05Skin Discoloration Near the AnkleBrownish or reddish staining of the skin near the ankle indicates that red blood cells are leaking from overpressured veins into surrounding tissue. Because this reflects advanced, sustained vein damage, it demands prompt evaluation without delay.

Who Is at Higher Risk
Venous insufficiency is more common than most people realize, and certain factors substantially increase the likelihood of developing it. Furthermore, many of these risk factors are everyday occupational and lifestyle habits that accumulate damage quietly over years.
"Achy legs on a Monday are not a sign of weakness. They are a sign that your veins have been working against pressure all week, and that the source of that pressure deserves proper attention."
What You Can Do to Reduce the Aching
While no lifestyle change can reverse valve damage that has already occurred, the following measures can nonetheless reduce daily venous pressure and slow the progression of vein disease in the meantime. Implementing these consistently, particularly on working days, makes a measurable difference.
These measures help manage symptoms, but they do not correct the underlying valve damage. If your legs ache on a predictable weekly basis, a vein evaluation is the most important step you can take. A vein specialist can confirm whether venous insufficiency is present using a simple, painless duplex ultrasound and outline the most direct path to lasting relief.
Treatments That Actually Solve the Problem
Modern vein treatment no longer means surgery, hospital admission, or weeks of recovery. Today, all major procedures are minimally invasive, performed in-office under local anesthetic, and allow patients to return to normal activity the same day. Furthermore, long-term success rates are high and the procedures are well tolerated.
Since the appropriate treatment depends on the size and location of the affected veins, your specialist will evaluate these factors during a duplex ultrasound before making a recommendation.
Minimally Invasive Options Your Specialist May Recommend
A thin catheter delivers controlled heat along the diseased vein, causing it to collapse and seal permanently. As a result, blood reroutes naturally through healthy surrounding vessels. Notably, RFA carries a success rate above 92% with same-day recovery, making it one of the most widely used procedures available. Learn about RFA.
A medical solution injected directly into the affected vein causes it to scar and close permanently. This approach is particularly effective for smaller varicose veins and spider veins. Furthermore, multiple veins can be treated in a single session with no anesthesia required, and most patients notice clear improvement within a few weeks.
A medical-grade adhesive is delivered into the diseased vein, bonding the walls together and closing it permanently. Unlike thermal techniques, VenaSeal requires no heat, no tumescent anesthesia, and no post-procedure compression stockings, making it one of the most comfortable options currently available.
A rotating catheter tip combines mechanical disruption of the vein wall with a chemical sclerosant, achieving permanent closure without thermal energy. It is therefore an excellent option for patients who cannot tolerate tumescent anesthesia. For a full comparison of these approaches, this overview of top vein treatments covers all the key differences.
Monday Shouldn't Feel Like This
A duplex ultrasound is all it takes to find out whether vein disease is behind your symptoms. In most cases, the consultation is straightforward, painless, and covered by insurance when symptoms are documented.
Book a Consultation
