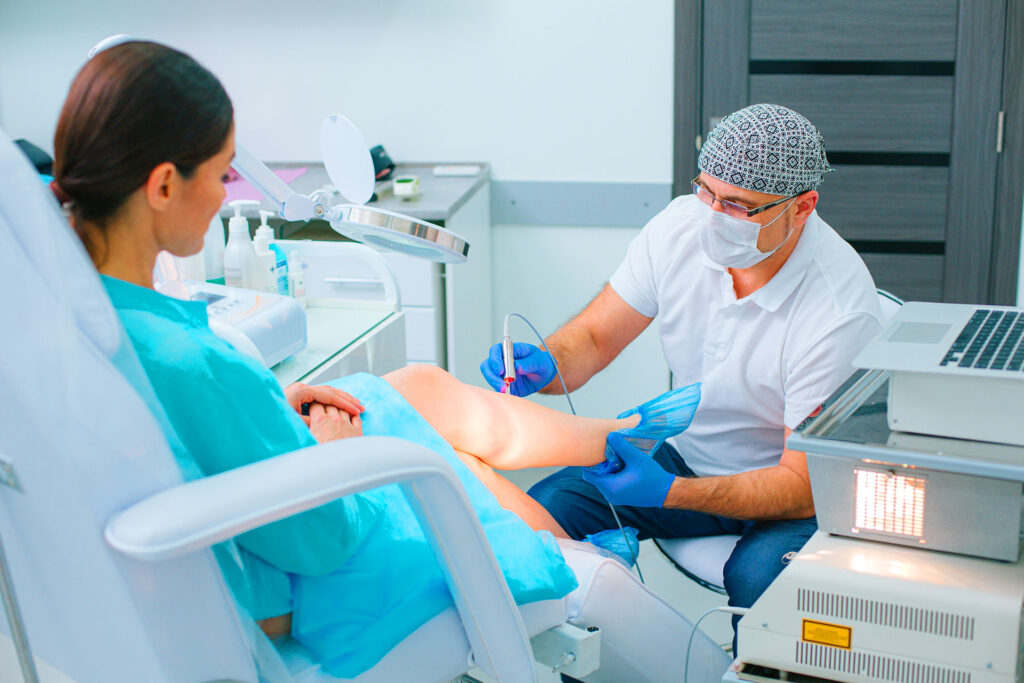
Vein disease is far more common than most people realize. If you have been noticing heavy legs, visible varicose veins, or persistent swelling, a vein clinic visit could be the first step toward lasting relief. This guide walks you through who should consider going, what the evaluation process involves, and what treatment options are available.
Who Should Consider Visiting a Vein Clinic?
Your veins carry blood back to the heart through a system of one-way valves. When those valves weaken or fail, blood flows backward and pools in the lower legs, a condition known as chronic venous insufficiency. Several risk factors can contribute, including genetics, advancing age, a history of blood clots, prolonged sitting or standing, obesity, and pregnancy.
Common Signs and Symptoms
Leg Heaviness
A persistent tiredness or pressure in the legs, especially after long periods of standing.
Leg Pain and Aching
Dull, throbbing pain in the calves or thighs that worsens as the day progresses.
Night Cramps
Involuntary leg cramps during sleep, often linked to poor venous circulation.
Swelling (Edema)
Swelling in the ankles and lower legs, particularly noticeable at the end of the day.
Varicose Veins
Bulging, twisted veins visible beneath the skin surface, often appearing on the legs.
Skin Changes
Discoloration, surface eczema, or in advanced cases, venous skin ulcers.
Left untreated, chronic venous insufficiency can progress from mild discomfort to serious skin changes and ulceration. Early evaluation by a board-certified vein specialist is the most effective way to prevent long-term complications.
What Happens During Your Vein Clinic Visit?
A vein clinic visit follows a structured, step-by-step process designed to give your physician a complete picture of your venous health before recommending any treatment.
Consultation with a Board-Certified Phlebologist
Your visit begins with a thorough consultation with a vein specialist, also known as a phlebologist. Qualified phlebologists hold certifications in disciplines such as vascular surgery, cardiology, or through the American Board of Venous and Lymphatic Medicine (ABVLM). Verifying these credentials before your visit is always a smart first step.
Medical History Review and Physical Examination
The specialist will take a detailed medical history, ask about your symptoms, lifestyle, and family history of vein disease, and perform a physical examination of your legs. This helps identify risk factors and determine which diagnostic tests are appropriate.
Vascular Duplex Ultrasound
In most cases, a registered vascular technologist will perform a non-invasive duplex ultrasound of your legs. This imaging study maps the venous system, identifies points of valve failure and reflux, and measures the severity of any insufficiency. Look for clinics whose sonographers hold the Registered Vascular Technologist (RVT) credential from the American Registry for Diagnostic Medical Sonographers (ARDMS).
Results Review and Personalized Treatment Plan
Once testing is complete, your physician will review the findings with you and outline a personalized treatment plan. The recommended approach will depend on the size and location of affected veins, your symptoms, and personal goals. Most treatments are performed in-office and covered by insurance when medically indicated.
Available Vein Treatment Options
Modern vein clinics offer a range of minimally invasive procedures for both medical and cosmetic vein conditions. Your specialist will recommend the approach that best fits your anatomy and goals.
Endovenous Thermal Ablation
Ultrasound-Guided Foam Sclerotherapy
Surface Sclerotherapy
Frequently Asked Questions
Still have questions about what to expect from a vein clinic? Our specialists answer the most common ones below.
In many cases, yes. When varicose veins cause documented medical symptoms such as pain, swelling, or skin changes, treatment is typically considered medically necessary and covered by most major insurance plans. Purely cosmetic procedures such as surface sclerotherapy for spider veins are generally not covered. Our team at CURA will verify your benefits before your visit so there are no surprises.
An initial consultation, including the physical exam and vascular ultrasound, typically takes between 60 and 90 minutes. Treatment appointments are usually shorter. Most in-office procedures such as thermal ablation or sclerotherapy are completed within 30 to 60 minutes, after which patients can return to light daily activities the same day.
Not at all. A vascular duplex ultrasound is completely non-invasive and painless. A small handheld probe is moved along the surface of your leg to produce images of the veins beneath the skin. No needles, no radiation, and no preparation is required beforehand. Most patients find it similar to a standard imaging exam.
Look for physicians who are board-certified through the American Board of Venous and Lymphatic Medicine (ABVLM) or who hold certification in vascular surgery or cardiology. For the ultrasound team, the Registered Vascular Technologist (RVT) credential from ARDMS is the benchmark standard. At CURA Vein Centers, all treating physicians and sonographers hold the appropriate credentials.
This depends on the extent and severity of your vein disease. Some patients achieve their goals in a single session, while others with more widespread insufficiency may require a series of treatments over several weeks. Your physician will give you a clear treatment timeline during your consultation, based on your ultrasound findings and symptom profile.
Treated veins do not return. However, vein disease is a chronic condition, and new veins can develop over time, particularly if underlying risk factors such as genetics, prolonged standing, or hormonal changes are still present. Wearing compression stockings, maintaining a healthy weight, and staying active can all help slow the progression of new vein disease after treatment.