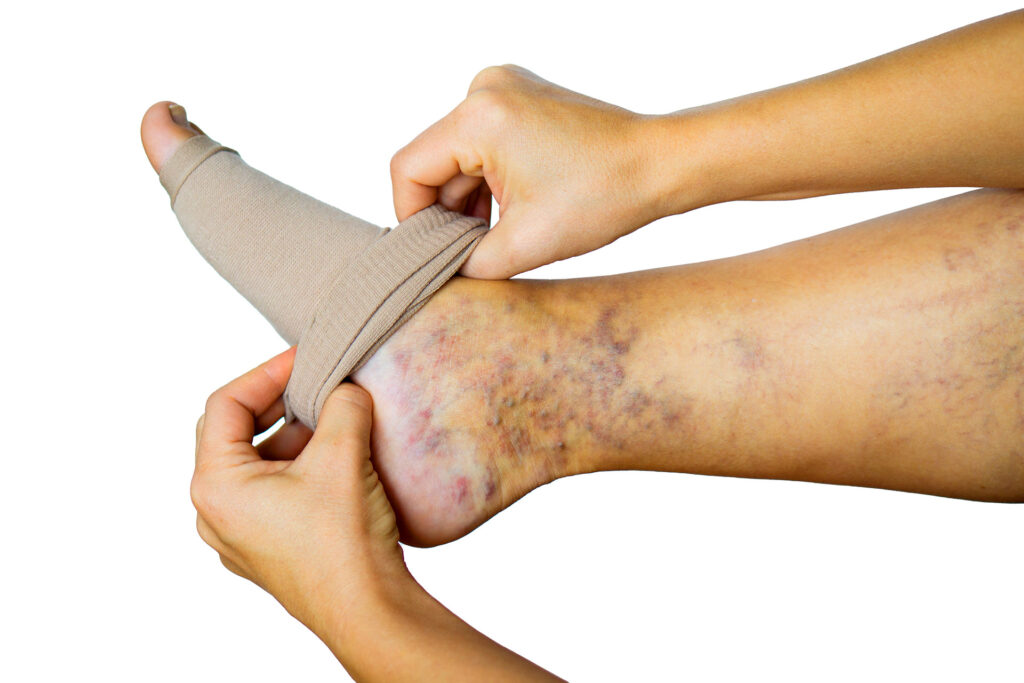
If you’ve been dealing with bulging, twisted veins on your legs, you’ve probably wondered whether support socks for varicose veins can actually make a difference. The short answer? Yes, and they might just be one of the most affordable, non-invasive tools in your vein health arsenal. Whether you’re standing all day at work, sitting on long flights, or simply looking for relief from aching, swollen legs, the right pair of compression socks can transform how your legs feel by the end of the day.
What Are Support Socks for Varicose Veins?
Support socks, also commonly known as compression stockings or compression socks, are specially designed garments that apply graduated pressure to your legs. The compression is strongest at the ankle and gradually decreases as it moves up the leg, helping push blood back toward your heart.
Unlike regular socks, these medical-grade garments are engineered with specific pressure levels measured in millimeters of mercury (mmHg). They’re a frontline solution recommended by vein specialists worldwide for managing varicose veins, spider veins, and chronic venous insufficiency.
How Do They Work?
Varicose veins develop when the tiny valves inside your veins weaken or fail, allowing blood to pool instead of flowing efficiently back to the heart. Support socks counteract this by:
- Squeezing the leg muscles to promote upward blood flow
- Reducing vein diameter, which helps faulty valves close more effectively
- Decreasing swelling by preventing fluid buildup in the lower legs
- Improving oxygen delivery to leg tissues
- Preventing blood clots, especially during long periods of inactivity

Who Should Wear Support Socks?
Compression socks aren’t just for people who already have visible varicose veins. They benefit a wide range of individuals, including:
- People with existing varicose or spider veins
- Pregnant women (especially in the second and third trimesters)
- Nurses, teachers, retail workers, and others who stand for long hours
- Office workers who sit at a desk all day
- Frequent travelers, particularly on long flights
- Athletes recovering from intense workouts
- Individuals with a family history of vein disease
- Post-surgical patients at risk of deep vein thrombosis (DVT)
Important Note: While support socks provide excellent symptom relief, they don’t cure varicose veins. If your symptoms persist or worsen, it’s crucial to consult a vein specialist for a comprehensive evaluation.
Understanding Compression Levels
Choosing the right compression level is essential, too little won’t provide benefits, while too much can cause discomfort or circulation issues. Here’s a breakdown of the main categories:
Mild Compression (8–15 mmHg)
Best for everyday wear, mild leg fatigue, and prevention. Ideal for those who sit or stand for moderate periods.
Moderate Compression (15–20 mmHg)
Great for travel, pregnancy, mild varicose veins, and minor swelling. This is the most popular over-the-counter option.
Firm Compression (20–30 mmHg)
Recommended for moderate to severe varicose veins, post-surgical recovery, and managing chronic venous insufficiency. Often requires a doctor’s recommendation.
Extra Firm Compression (30–40 mmHg)
Used for severe varicose veins, lymphedema, and serious venous disorders. A prescription is typically required.
Key Benefits of Wearing Support Socks
The advantages of consistent compression sock use go far beyond simple comfort. Many users report dramatic improvements in their daily quality of life within just a few weeks.
- Reduced leg pain and heaviness after long days
- Less swelling in feet and ankles
- Decreased risk of blood clots during travel or bed rest
- Slowed progression of existing varicose veins
- Faster muscle recovery after exercise
- Improved energy and reduced fatigue in the legs
- Prevention of new varicose veins from forming

Why Ignoring Varicose Veins Is Risky
Many people dismiss varicose veins as merely a cosmetic concern, but untreated vein disease can lead to serious health complications. From skin ulcers and bleeding to potentially life-threatening blood clots, there are several hidden dangers of varicose veins that every patient should understand before deciding whether to seek treatment. Support socks are an excellent first-line defense, but they work best as part of a broader vein health strategy guided by a qualified specialist.
How to Choose the Right Support Socks
Not all compression socks are created equal. Here’s what to look for when shopping for your first pair:
1. Get Properly Measured
Sizing is critical. Measure your ankle, calf, and leg length first thing in the morning before any swelling occurs. Most reputable brands provide detailed sizing charts.
2. Choose the Right Length
- Knee-high: Most common; ideal for ankle and calf vein issues
- Thigh-high: Better for veins higher up the leg
- Pantyhose style: Best for varicose veins extending into the upper thighs or for pregnancy
3. Consider the Material
Look for moisture-wicking, breathable fabrics like nylon-spandex blends, merino wool, or bamboo. These reduce irritation and keep your legs comfortable all day.
4. Check the Fit
Support socks should feel snug but not painful. They should never roll down, pinch, or cut off circulation. If your toes turn blue or numb, the size or compression level is wrong.
Tips for Wearing and Caring for Your Socks
Wearing Tips
- Put them on first thing in the morning
- Apply lotion the night before, not the same morning
- Use rubber gloves for easier grip when pulling them up
- Smooth out wrinkles to prevent pressure points
- Wear them throughout the day, removing at bedtime
Care Tips
- Hand wash or use a gentle machine cycle
- Use mild detergent without bleach or fabric softener
- Air dry, avoid the dryer to maintain elasticity
- Replace every 3–6 months for optimal compression
- Rotate between two or three pairs to extend their lifespan
When to See a Vein Specialist
While support socks for varicose veins offer significant relief, they’re not a substitute for professional medical care. You should consult a vein specialist if you experience:
- Severe pain, throbbing, or cramping in your legs
- Skin discoloration or ulcers near the affected veins
- Bleeding from a varicose vein
- Sudden swelling in one leg (possible DVT)
- Veins that feel hard, warm, or tender to the touch
- Symptoms that don’t improve with compression therapy
Final Thoughts
Support socks for varicose veins are one of the simplest, most effective ways to manage symptoms, prevent progression, and improve your daily comfort. They work by enhancing blood flow, reducing swelling, and supporting weakened veins, though persistent localized nerve pain alongside varicose veins may signal a deeper issue worth investigating.
That said, support socks are just one piece of the puzzle. If your varicose veins are causing pain, affecting your quality of life, or showing signs of complications, don’t wait. Consult a board-certified vein specialist who can recommend a personalized treatment plan tailored to your unique needs. Your legs carry you through life; give them the care they deserve.