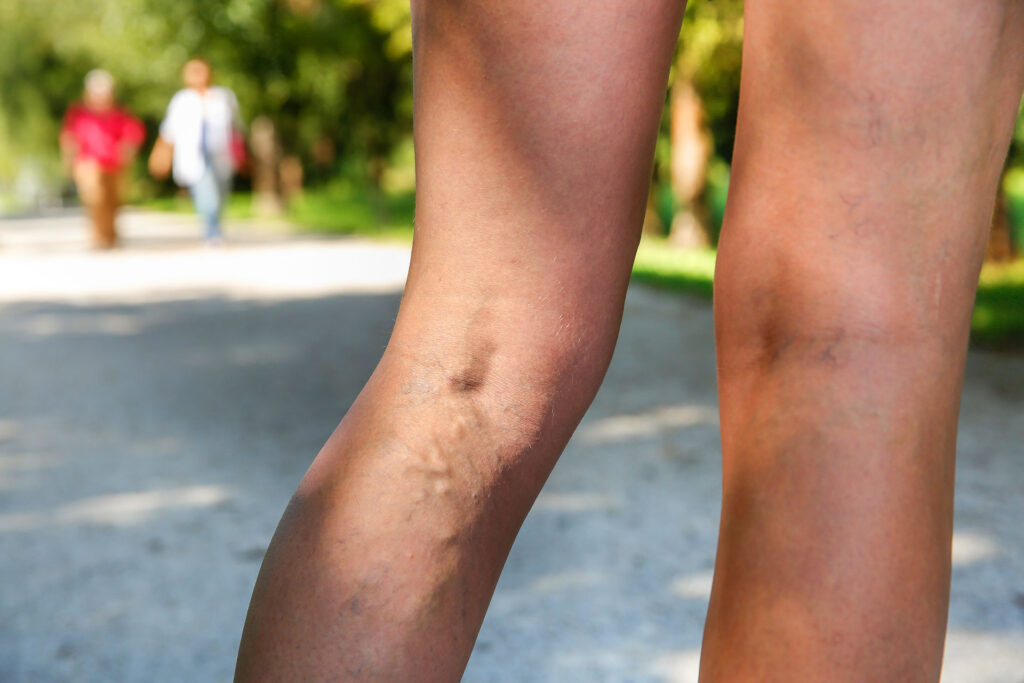
Nearly 2.5 million Americans live with venous insufficiency, and up to 20% will develop venous ulcers without proper management. While medical treatment is essential, everyday nutrition is one of the most powerful and accessible tools available for protecting your vein health at every stage of the condition.
Understanding Venous Insufficiency
Knowing what drives the condition helps you make smarter dietary choices.
Venous insufficiency occurs when the one-way valves inside the leg veins weaken or fail, allowing blood to flow backward and pool in the lower extremities rather than returning to the heart. This raises venous pressure, stretches vessel walls, and over time produces varicose veins, spider veins, leg swelling, skin discoloration, and in severe cases, venous ulcers. Risk factors divide into two categories:
🔒 Non-Modifiable Risk Factors
- Age and advancing years
- Genetics and family history
- Female hormones and hormonal changes
- Previous history of blood clots
✏️ Modifiable Risk Factors
- Diet and nutritional choices
- Body weight and obesity
- Sedentary lifestyle
- Smoking
- Prolonged standing or sitting
- Pregnancy
While dietary changes cannot reverse existing valve damage, they can meaningfully slow disease progression, reduce symptom severity, support healthy body weight, and protect the structural integrity of your vein walls. Combined with proper medical treatment, the right nutrition makes a real difference.
6 Dietary Strategies for Vein Health
Evidence-based nutritional choices to manage venous insufficiency symptoms and protect your veins.
Stay Hydrated for Healthy Circulation
Water is the foundation of healthy blood flow. The body is approximately 60% water, and adequate hydration is critical for maintaining the viscosity of blood. When you are dehydrated, blood thickens and becomes harder to move through the venous system, placing additional strain on already compromised valves. Staying hydrated helps flush metabolic waste, reduces blood pooling, and supports efficient venous return.
Aim for at least 8 glasses of water daily. Herbal teas, broths, and water-rich fruits and vegetables all contribute to your total fluid intake. Limit caffeine and alcohol, both of which have dehydrating effects that can worsen venous symptoms.
🍵 Herbal teas
🍉 Watermelon
🥒 Cucumbers
🍲 Broths
🍓 Berries
Reduce Sodium, Increase Potassium
Sodium and potassium are the two primary electrolytes governing blood pressure and fluid balance. Diets high in sodium are strongly linked to hypertension and fluid retention, both of which increase the pressure burden on your venous system. The recommended daily sodium intake is around 2 grams, yet most Americans consume significantly more through processed and packaged foods.
Potassium acts as a natural counterbalance. When potassium moves into cells, sodium moves out, helping to lower blood pressure and reduce excess fluid in the tissues.
✕ Limit or Avoid
- Processed and deli meats
- Chips and salty snacks
- Canned soups and goods
- Fast food and condiments
- Instant noodles and meals
- Aged cheeses
✓ Add to Your Plate
- Bananas and avocados
- Sweet potatoes
- Cooked spinach and broccoli
- Mushrooms and peas
- Beans and legumes
- Dried prunes and raisins
High-Fiber Foods for Weight and Vein Management
Dietary fiber supports vein health in two critical ways. First, it aids weight management by increasing satiety and reducing overall caloric intake. Excess body weight places sustained upward pressure on the venous system, accelerating valve deterioration and amplifying symptoms. Second, fiber prevents chronic constipation, which reduces straining that raises intra-abdominal pressure and directly impedes blood return from the lower legs.
✓ Insoluble Fiber
- Whole wheat bread and pasta
- Bran and wheat germ
- Flaxseeds
- Green beans and peas
- Brown rice
✓ Soluble Fiber
- Oats and oat bran
- Apples and citrus fruits
- Carrots and sweet potatoes
- Barley and legumes
- Berries
Flavonoids: Nature’s Vein-Strengthening Compounds
Flavonoids are plant-based compounds with potent antioxidant and anti-inflammatory properties. They neutralize free radicals, strengthen capillary walls, reduce vascular permeability, and improve blood flow. Research has linked flavonoid-rich diets to reduced capillary fragility, less fluid leakage into surrounding tissues, and decreased leg discomfort and edema in patients with venous insufficiency.
For patients dealing with spider veins, flavonoids are a particularly relevant dietary tool given their role in strengthening superficial capillary walls. Add variety and color to your plate to boost your intake of these vein-protective compounds.
🍓 Strawberries
🍊 Citrus fruits
🍎 Apples
🫑 Bell peppers
🥦 Broccoli
🍵 Green tea
🍫 Dark chocolate
🧅 Red onions
🥬 Leafy greens
Anti-Inflammatory Foods for Vascular Protection
Chronic inflammation is a key driver of vascular disease progression, damaging vessel walls and accelerating vein valve breakdown. Adopting a broadly anti-inflammatory dietary pattern, such as the Mediterranean diet, is one of the most evidence-supported nutritional strategies for vein and cardiovascular health.
✕ Promote Inflammation
- Refined sugars and sweets
- Ultra-processed foods
- Trans fats and fried foods
- Refined white flour products
- Excessive alcohol
✓ Reduce Inflammation
- Salmon, mackerel, sardines
- Extra virgin olive oil
- Walnuts and almonds
- Turmeric and ginger
- Tomatoes and colorful vegetables
Vitamin C and Collagen for Vein Wall Integrity
Vitamin C serves a dual function in vein health. As an antioxidant, it combats oxidative stress that degrades vessel walls. As an essential cofactor in collagen synthesis, it maintains the structural strength and elasticity of veins and surrounding connective tissue. Strong, flexible vein walls are better equipped to withstand the elevated pressures associated with venous insufficiency.
For patients seeking vein treatment specialists in Wayne, New Jersey, understanding how nutrition supports post-treatment recovery and long-term vein health is an important part of the overall care plan.
🍊 Citrus fruits
🍓 Strawberries
🥝 Kiwi
🥦 Broccoli
🍅 Tomatoes
🍖 Bone broth
🥬 Leafy greens
Dietary changes are a valuable complement to proper medical care, not a substitute. If you are experiencing symptoms of venous insufficiency including visible varicose or spider veins, leg heaviness, persistent swelling, or skin changes, a consultation with a board-certified vein specialist is the essential next step.
Frequently Asked Questions
Common questions about diet, nutrition, and venous insufficiency answered by our specialists.
No dietary change can reverse existing vein valve damage or cure venous insufficiency. However, the right nutritional choices can meaningfully slow disease progression, reduce the severity of symptoms such as swelling and leg heaviness, help maintain a healthy body weight, and support the structural integrity of your vessel walls. Diet works best as part of a comprehensive management plan that includes medical evaluation and, when appropriate, minimally invasive treatment.
The foods most harmful to vein health are those high in sodium, refined sugars, trans fats, and inflammatory compounds. This includes ultra-processed foods, fast food, fried foods, salty snacks, cured and deli meats, sweetened beverages, and refined white flour products. These foods promote fluid retention, elevated blood pressure, inflammation, and weight gain, all of which worsen venous insufficiency symptoms and accelerate vascular disease progression.
Flavonoids strengthen the walls of capillaries and small blood vessels, reducing their permeability and fragility. In patients with venous insufficiency, this translates to less fluid leaking out of the veins into surrounding tissue, which reduces edema. Some flavonoids also have mild anti-inflammatory effects on vessel walls and may help ease the aching and discomfort associated with varicose veins. They are a complementary measure rather than a primary treatment, but a genuinely useful one.
Yes. Proper hydration helps maintain healthy blood viscosity, making it easier for blood to travel through the venous system. Dehydration causes blood to thicken, which increases the workload on already weakened vein valves and raises the risk of blood pooling and clot formation. Staying well hydrated also supports the overall efficiency of the circulatory system and can help reduce the visible symptoms of mild venous congestion.
Some supplements have shown promise for vein health in clinical research, including horse chestnut seed extract, diosmin and hesperidin, and Pycnogenol. However, supplements should never replace a balanced diet or medical treatment. Always consult your physician before adding any supplement to your routine, particularly if you are taking blood thinners or other medications. Whole food sources remain the most reliable and safest approach for most patients.
Excess body weight places sustained additional pressure on the venous system in the lower legs, accelerating the deterioration of vein valves and worsening the symptoms of venous insufficiency. Patients who achieve and maintain a healthy weight through diet and exercise typically experience a meaningful reduction in leg heaviness, swelling, and discomfort. Weight management is one of the highest-impact lifestyle changes available to patients managing vein disease.