What Sets Spider Veins Apart?
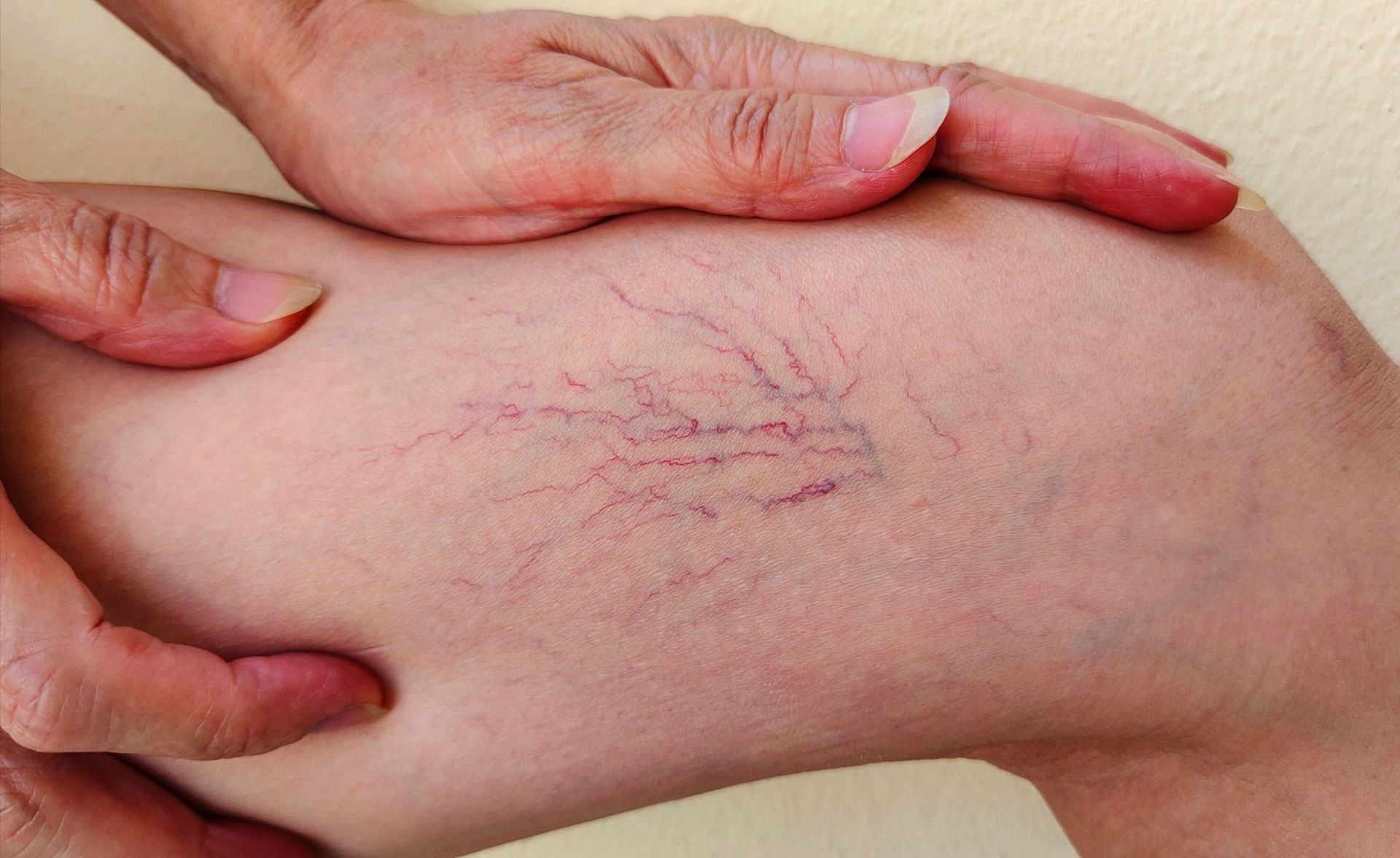
Spider veins are small blood vessels often appearing on the skin’s surface. Spider veins
are smaller in size than varicose veins and are located closer to the surface of the skin. They
can appear anywhere on the body but are most often found on the legs and face.
Twisted Veins and Spider Veins
Twisted veins, also known as spider veins, are tiny blood vessels near the surface of the skin. These veins get their name because they often look like intricate spider webs or twisted tree branches.
Spider veins are usually small and can be red, blue, or purple. They commonly appear on the legs but can also be found on the face or other body parts.
While they are generally harmless and don’t cause pain, they can be a cosmetic concern for some people.
Factors like genetics, prolonged standing, or hormonal changes can contribute to spider vein development.
Symptoms of Spider Veins
Symptoms of spider veins are primarily visual, such as small blood vessels.
While spider veins rarely cause physical discomfort, some individuals may experience aching or a heavy feeling in the legs, particularly after long-standing.
In some instances, the affected area may become tender to the touch.
Early intervention can help prevent the development of new spider veins and address any underlying issues.
Treatment Options
Lifestyle Changes
Lifestyle changes to prevent existing spider veins from worsening include:
- Maintaining a healthy weight
- Exercising regularly
- Avoiding long periods of sitting or standing
Laser Therapy and Intense Pulsed Light (IPL)
Laser treatment can effectively reduce the appearance of spider veins by targeting the affected vessels.
Laser therapy and Intense Pulsed Light (IPL) are advanced non-invasive treatments used in dermatology and vascular medicine. In the context of vein-related issues like varicose veins and spider veins, laser therapy involves the use of focused laser beams to target and treat problematic veins.
Sclerotherapy
During the procedure, a solution known as a sclerosant is injected directly into the affected veins. This solution irritates the vein walls, causing them to stick together and eventually close off.
Sclerotherapy is particularly effective for treating spider veins. The procedure helps improve blood flow by redirecting it to healthier veins.
While larger varicose veins may require alternative treatments, sclerotherapy is an excellent option for addressing small blood vessels and preventing the development of new spider veins.
Wearing compression stockings is recommended post-treatment to enhance the effectiveness of sclerotherapy and reduce potential side effects like leg swelling or discomfort. Sclerotherapy provides a non-surgical solution for improving the appearance and health of affected vein.
In sclerotherapy, a specialized solution is injected into the affected vein, causing it to collapse and gradually disappear.
Conclusion
Understanding spider veins involves recognizing their causes, symptoms, and available treatments. By implementing preventive measures and seeking medical advice, patients can manage and address this common vascular concern.
Whether through lifestyle changes or medical interventions, there are options to improve the appearance and alleviate symptoms associated with varicose or spider veins.